Specialized, comprehensive treatment for acute and chronic leukemia
Leukemia refers to a group of cancers that develop in the bone marrow, the soft inner part of bones where new blood cells are made. When white blood cell DNA is altered, the abnormal cells begin to multiply, which slows down the production of healthy white and red blood cells and platelets.
This type of blood cancer can be acute (develops quickly) or chronic (develops slowly over time), and there are many different subtypes, each requiring a unique approach to treatment. While many other cancers frequently affect adults, this disease is the most common cancer in children and teens, accounting for one of three cases. Fortunately, we can cure more and more patients as research continues on innovative, promising therapies.
Symptoms and risk factors
What are the signs of leukemia?
Typically, signs of acute leukemia appear suddenly, while patients with chronic leukemia may not show symptoms for several years. As leukemic cells begin to overcrowd the bone marrow, symptoms may include:
-
Fever or night sweats
-
Easy bruising or bleeding
-
Petechiae (flat, pinpoint, dark-red spots under the skin caused by bleeding)
-
Weakness, fatigue, or pale appearance
-
Unexplained weight loss or loss of appetite
-
Shortness of breath (adults)
-
Bone or joint pain
-
Painless lumps in the neck, underarm, stomach, or groin
-
Pain or feeling of fullness below the ribs
-
Getting many infections
Other conditions can cause similar symptoms, too, so it’s important to see a doctor for a proper diagnosis.
We don’t know what causes most cases of leukemia, but certain risk factors can increase your chances of developing the disease.
Risk factors vary for each common type of leukemia and may include:
-
Risk factors for acute Lymphocytic leukemia (ALL)
Risk factors for ALL include:
- Age: Children have the highest risk for developing ALL, usually before age five. (Two-thirds of cases occur in children and teens.) The risk declines until the mid-20s, levels off, and slowly rises again after 50.
- Race/Ethnicity: In adults, ALL is more common in whites than African-Americans.
- Previous treatments: Past chemotherapy or radiation treatment can increase your risk.
-
Inherited syndromes: While ALL itself does not seem to run in families, certain inherited genetic syndromes can raise the risk of developing the disease:
- Down syndrome
- Klinefelter syndrome
- Fanconi anemia
- Bloom syndrome
- Ataxia-telangiectasia
- Neurofibromatosis
-
Risk factors for acute myeloid leukemia (AML)
Risk factors for AML include:
- Age: AML rarely strikes before age 45, as 66 is the average patient age.
- Smoking: Smoking can increase your risk, as can secondhand exposure to smoke.
- Previous treatments: Past treatment with chemotherapy or radiation can increase your risk, as can previous treatment for childhood ALL.
- Chemicals: Benzene exposure can increase your risk.
- Blood disorders: You may face a greater risk if you have a history of blood disorders such as aplastic anemia or myelodysplastic syndrome.
-
Genetic disorders: Certain genetic disorders can increase your risk, including:
- Down syndrome
- Fanconi anemia
- Neurofibromatosis type 1 (NF1)
- Noonan syndrome
- Shwachman-Diamond syndrome
-
Risk factors for chronic lymphocytic leukemia (CLL)
There are known risk factors for CLL:
- Age: CLL is rarely seen before age 40, as 72 is the average age of diagnosis.
- Family history: A family history of CLL, or lymph system cancer, increases your risk.
- Ethnicity: You may have a higher risk if you are Jewish and your family came from Russia or Eastern Europe.
-
Risk factors for chronic myeloid leukemia (CML)
The only known risk factor for CML is age. The disease mainly affects adults, with 64 as the average age at diagnosis.
Screening and prevention
Can leukemia be prevented?
No, there is no clear way to prevent these types of cancers in either adults or children. However, several lifestyle changes may lower your risk of all cancers, such as:
-
Avoiding or quitting smoking
-
Maintaining a healthy weight
-
Avoiding certain harmful chemicals, such as benzene or formaldehyde
Diagnosis
Successful treatment depends on a complete and accurate diagnosis.
Each of our patients receives a thorough evaluation so we can create an individualized plan. Because there are several types of leukemia, understanding any specific genetic alterations is vital so we can determine the best treatment approach.
Typically, we diagnose leukemia with the following:
-
History and physical examination: We conduct a thorough examination and ask comprehensive questions about your full personal and family medical history.
-
Blood work: We may take a blood sample to test your complete blood count (CBC), blood chemistry, and other factors.
-
Biopsy: We use a hollow needle to remove a small sample of bone marrow, blood, and bone from the hip bone or breastbone. The samples are studied under a microscope and may get other testing, including analysis for genetic changes.
After collecting blood and tissue samples, our hematopathologists thoroughly analyze them to identify the molecular profile of the leukemia cells. We may also conduct additional testing to confirm the type and determine whether it has spread. These tests may include:
-
Chest x-ray: Low-dose radiation is used to take pictures of the chest.
-
CT (CAT) scan: Computed tomography takes a series of X-rays from different angles, then stitches them together into 3D images.
-
MRI: Magnetic resonance imaging uses a powerful magnetic field and radio waves to create detailed 3D images at higher contrast than CT scans which can be useful for clarifying other test results.
-
Lumbar puncture (LP, or Spinal Tap): A needle is inserted into the spinal column to take a sample of cerebrospinal fluid.
-
Biopsy of testicles, ovaries, or skin: A needle is used to remove cells or tissues if the cancer has caused changes to the testicles, ovaries, or skin, and the samples are checked under a microscope.
Types of cancer
Leukemia is classified by the type of white blood cell involved and how quickly it develops.
Each type has different characteristics—the kind of cells they start in, their growth rate, how they are treated, and whether they are found mainly in adults, teens, or children.
It develops from the two types of bone marrow stem cells:
-
Lymphoid stem cells, which turn into lymphoblasts and then most infection-fighting white blood cells (lymphocytes)
-
Myeloid stem cells, which turn into oxygen-carrying red blood cells, clot-forming platelets, and another type of white blood cell
Cancer causes too many cells to form, and they don’t mature. This means they fail to function properly and also crowd out other cells the body needs. The cancers also take one of two forms, based on how quickly they develop:
-
Acute: The immature cells quickly build up and kill most patients within months if the disease is not treated.
-
Chronic: The cancer progresses more slowly, giving most people longer to live, but usually proving harder to treat than acute cases. Chronic leukemia is rare in children and teens.
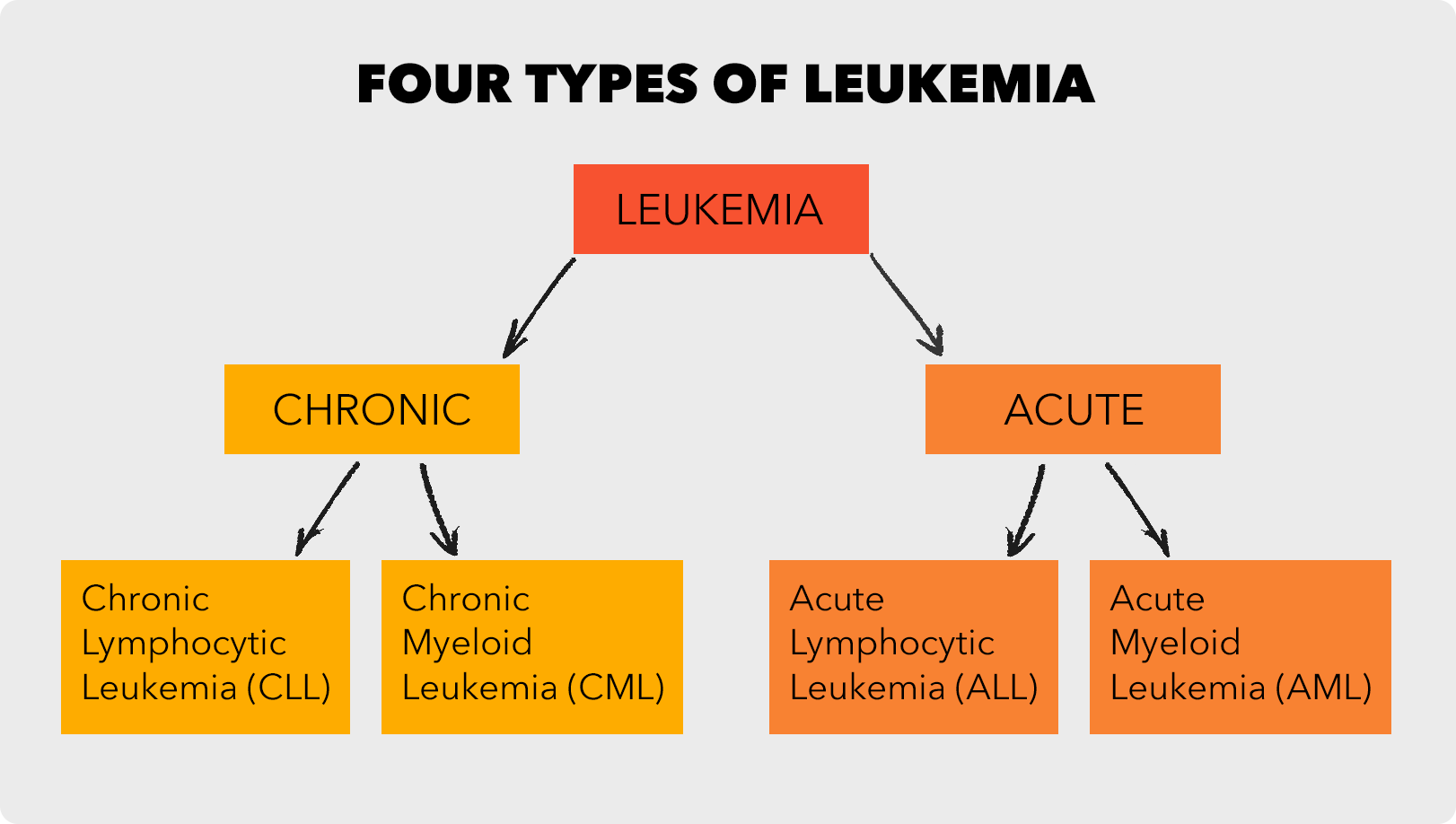
Combining the type of stem cell with the rate of growth gives the four main types of leukemia:
-
Acute lymphocytic leukemia (ALL):
- Most pediatric leukemia is ALL (three out of four cases)
- Least common type among adults
- Can spread to the central nervous system (brain and spinal cord)
-
Acute myeloid leukemia (AML):
- Represents most of the remaining pediatric leukemia cases
- Relapses more frequently than ALL
-
Chronic lymphocytic leukemia (CLL):
- Mainly affects older adults, as the average age at diagnosis is around 72
- Rarely curable but most patients live with it for many years
- Might not need treatment right away, but usually need it eventually
-
Chronic myeloid leukemia (CML):
- Mainly affects adults—average age at diagnosis is around 64
- Treatment doesn’t usually cure the disease, but keeps it in check
Each main type of leukemia also has subtypes that often play a role in disease progression and treatment recommendations.
Treatments
Leukemia treatment depends on the cell type, speed of progression, your age, and overall health.
We take a comprehensive approach to treating this blood cancer with input from a multidisciplinary team. Through weekly tumor boards, experts in chemotherapy, targeted therapy, stem cell transplantation, and cellular immunotherapy collaborate on the best way to treat your leukemia based on its genetic makeup.
Our recommendations for the best treatment approach for adults typically depend on the following:
-
Leukemia type: ALL, AML, CLL or CML
-
Type of cells the cancer began in and the leukemia subtype, as patients with different subtypes may have different prognoses and responses to treatment
-
Patient’s age and overall health
-
The presence of certain genetic changes, including the Philadelphia chromosome
-
If the leukemia is newly diagnosed or has come back (a relapse)
-
Number of immature cells versus healthy red blood cells, white blood cells and/or platelets
-
Whether the patient received chemotherapy in the past for a different cancer
-
Whether there is a history of a blood disorder like myelodysplastic syndrome
-
How quickly and how well the disease responds to initial treatment
-
Size of the spleen (CLL and CML only)
-
Size of the liver or lymph nodes (CML only)
-
Whether the leukemia was likely caused by previous cancer treatment (AML only)
Chemotherapy
Chemotherapy is a common treatment for acute subtypes of this disorder. It's commonly given in the hospital as the initial treatment for patients with ALL or AML. The goal of this approach is to kill as many cancerous cells as possible and put the disease in remission, which means getting rid of any evidence of the disease. It's often followed by consolidation or maintenance chemotherapy, which is designed to ensure any remaining leukemia cells are destroyed.
Stem cell transplants and CAR T-cell therapy
Some patients with acute and chronic leukemia benefit from stem cell transplantation after other cancer treatment. Transplantation replaces damaged stem cells with healthy ones using cells from the patient's bloodstream (autologous) or a donor (allogeneic).
MedStar Health is the largest stem cell collection center in the nation and the only adult program accredited by the Foundation for the Accreditation of Cellular Therapy (FACT) in Washington, D.C. With decades of experience, our dedicated bone marrow transplant specialists, nurses, and staff have exceptional expertise in these life-saving treatments.
Immunotherapy and targeted therapy
For patients with subtypes of chronic leukemia, we offer the full range of targeted therapies that are very effective. Most of these treatments are given orally through a pill and are considered less toxic than chemotherapy. These innovative therapies can target specific characteristics of certain leukemic cells, which is why an accurate diagnosis and genetic profiling of blood cancer cells is so important. The type of targeted therapy we recommend will vary based on the molecular makeup of a patient's cancer but may include the following, among others:
-
Tyrosine kinase inhibitors (TKIs): TKIs target the gene BCR-ABL, which is formed by an abnormal chromosome (the Philadelphia mutation) and makes a protein that helps cancer grow. TKIs are the main treatment for chronic myeloid leukemia (CML) and are also used for some acute lymphoblastic leukemia (ALL) patients who have the mutation.
-
Monoclonal antibody: These drugs replicate a natural antibody and target certain substances on cancer cells either alone or with a drug, toxin, or radioactive material to kill the cells, block their growth, or keep them from spreading.
-
FLT3 inhibitors: These drugs target mutations in the FLT3 gene in patients with acute myeloid leukemia (AML).
Looking for expert cancer care?
With multiple locations throughout the region, patients have access to many of the nation’s renowned cancer specialists offering high quality care, second opinions and a chance for better outcomes close to where they live and work. Georgetown Lombardi Comprehensive Cancer Center, one of the nation’s comprehensive cancer centers designated by the National Cancer Institute (NCI), serves as the research engine allowing patients access to clinical trials that often lead to breakthroughs in cancer care.
Our providers
Location: Change location Enter your location
Acute leukemia providers
-
Hira Latif, MD
Hematology Oncology
-
Kamyar Nader, MD
Myeloma, Lymphoma, Leukemia, Hematology & Hematologic Malignancy
-
Aarthi Ganesh Shenoy, MD
Hematology
-
Hedy P. Smith, MD,PhD
Hematology
-
Alaa Ali, MD,MSC
Cellular Therapy, Hematology & Medical Oncology
-
Kimberley R. Doucette, MD,MSC
Hematology Oncology
-
Kieron M Dunleavy, MD
Lymphoma, Hematology, Cellular Therapy & Medical Oncology
-
Anne Renteria, MD
Hematologic Malignancy & Hematology Oncology
-
Gustavo Adolfo Rivero, MD
Hematology Oncology
Chronic leukemia providers
-
Ravi Krishnan Anandakrishnan, MBBS
Medical Oncology
-
Kevin Y. Chen, MD
Medical Oncology & Hematology Oncology
-
Gurdeep Singh Chhabra, MD
Medical Oncology
-
Shweta Kurian, MD
Hematology Oncology & Medical Oncology
-
Hira Latif, MD
Hematology Oncology
-
Ankit Madan, MD
Hematology & Medical Oncology
-
Kathan D Mehta, MBBS, MPH
Hematology Oncology
-
Kamyar Nader, MD
Myeloma, Lymphoma, Leukemia, Hematology & Hematologic Malignancy
-
Charles A. Padgett, MD
Medical Oncology
-
Minal M. Shah, MD
Hematology & Hematology Oncology
-
Aarthi Ganesh Shenoy, MD
Hematology
-
Hedy P. Smith, MD,PhD
Hematology
-
Alaa Ali, MD,MSC
Cellular Therapy, Hematology & Medical Oncology
-
Kieron M Dunleavy, MD
Lymphoma, Hematology, Cellular Therapy & Medical Oncology
-
Anne Renteria, MD
Hematologic Malignancy & Hematology Oncology
-
Joseph Lee Roswarski, MD
Lymphoma, Hematology, Cellular Therapy & Medical Oncology
Our locations
Acute leukemia locations
Distance from my location Change location
MedStar Georgetown Cancer Institute at MedStar Washington Hospital Center
110 Irving Street, NW
Washington, D.C., 20010
MedStar Georgetown Cancer Institute at MedStar Georgetown University Hospital
3800 Reservoir Rd. NW
Washington, DC 20007
Chronic leukemia locations
Distance from Change locationEnter your location
MedStar Georgetown Cancer Institute at MedStar Georgetown University Hospital
3800 Reservoir Rd. NW Washington, DC 20007
MedStar Georgetown Cancer Institute at MedStar Washington Hospital Center
110 Irving Street, NW Washington, D.C., 20010
MedStar Health: MedStar Georgetown Cancer Institute at MedStar Montgomery Medical Center
18105 Prince Philip Dr. TG100 Olney, MD 20832
MedStar Georgetown Cancer Institute at MedStar St. Mary’s Hospital
25500 Point Lookout Rd. First Fl. Leonardtown, MD 20650
MedStar Georgetown Cancer Institute at MedStar Health Bel Air Medical Campus
12 MedStar Blvd. Ste. 180 Bel Air, MD 21015
MedStar Georgetown Cancer Institute at MedStar Franklin Square Medical Center
9103 Franklin Square Dr. The Harry and Jeanette Weinberg Cancer Institute Suite 220 Baltimore, MD 21237
MedStar Georgetown Cancer Institute at MedStar Southern Maryland Hospital
7501 Surratts Rd. Ste. 101 Clinton, MD 20735
MedStar Franklin Square Cancer Center at Loch Raven Campus
5601 Loch Raven Blvd. Russell Morgan Building First Floor Baltimore, MD 21239
Why choose us
-
Our world-renown doctors specialize in diagnosing and treating leukemia.
At MedStar Health, we have a dedicated team who focuses solely on diagnosing and treating patients with leukemia, including the rarest forms. This specialized expertise ensures we understand the optimal treatment options for each unique patient based on their leukemia type and stage, as well as their goals and preferences. The entire team of hematology oncologists, nurse practitioners, nurses, nurse navigators, and others are all committed to delivering you the best possible care with compassion.
-
We offer access to all of the latest leukemia treatments personalized to you.
Working as a team, our blood cancer experts customize treatment recommendations based on a precise diagnosis that pinpoints the unique characteristics of your cancer. This allows us to determine the right drugs and drug combinations for effective treatment, including novel therapies that are only available through clinical trials and advanced stem cell transplants, when appropriate. Through our research engine, the Georgetown Lombardi Comprehensive Cancer Center—the only of its kind in Washington, D.C., designated by the National Cancer Institute—our patients benefit from the latest breakthrough treatments before they become the standard of care.
-
We're the only Foundation for the Accreditation of Cellular Therapy (FACT)-accredited adult stem cell program in Washington, D.C.
If you would benefit from a stem cell transplant, we provide the complete spectrum of care, from cell collection and treatment to caring for any physical, emotional, and social needs you have throughout your journey. As the largest adult collection site in the country for the National Marrow Donor program, we have unmatched expertise in cell collection. In addition, our transplant specialists have decades of experience, allowing us to guide our patients safely through treatment and recovery.
Awards and recognition
Recipient of an Accreditation with Commendation, the highest level of approval, from the American College of Surgeons’ Commission on Cancer (CoC)
Numerous surgeons, medical oncologists, and radiation oncologists recognized as "Top Doctors" by both Baltimore Magazine and the Washingtonian
Magnet® designation from the American Nurses Credentialing Center (ANCC)
Clinical trials and research
Clinical trials
Clinical trials are studies that evaluate new treatments or treatment combinations to improve the standard of cancer care. Through this research, we learn better ways to target specific genetic alterations in leukemia cells, and we recommend participation in trials when they offer a personal benefit to our patients.
Research
The Georgetown Lombardi Comprehensive Cancer Center is MedStar Health's research engine propelling novel cancer treatment approaches. Our researchers and doctors continue investigating therapies that inhibit or kill leukemia cells, leveraging the body's own immune response, when possible.
Patient stories
Support services
If you or a loved one receives a leukemia diagnosis, we're here to support you through a full spectrum of services designed to care for your physical, emotional, and spiritual needs.
Genetic counseling
A small percentage of leukemias are linked to genetic disorders passed down from blood relatives, such as from parent to child. Our board-certified genetic counselors can help you determine whether or not genetic testing is right for you and your immediate family members. If it is, they'll thoroughly explain your results so you can make informed decisions about what to do with that information.
Personalized rehabilitation
Cancer treatment can lead to temporary or long-term side effects, and our specially trained physical and occupational therapists are here to help you fully recover. From nutritional counseling to personalized therapy plans that help you rebuild strength, stamina, and mobility, rehabilitation plays an essential role in your road back to good health.
Survivorship
After treatment, your care team will want to continue to monitor your health. Our comprehensive follow-up program is designed to help you manage any late side effects months and years after therapy. In addition, your check-ups may involve blood tests and imaging that will help to monitor for any signs of recurrence.